Borderless Benefits
A Third Party Administrator delivering capabilities to the insurance ecosystem across geographies and networks for over two decades
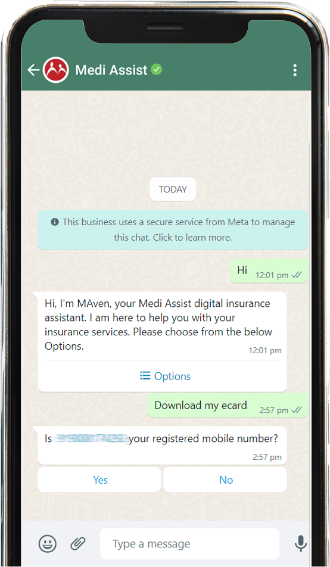
Introducing Medi Assist's New Avatar
A trusted companion who handles requests, removes obstacles, and provides seamless support, ensuring an effortless experience.

Our Expertise
Our digital-first technologies and integrated service capabilities seamlessly enhance member experiences
Our Footprint as of H1 - FY 25
Our vision & history
Incorporated in 2000, with a vision to deliver informed healthcare decisions to a billion lives connected by our technology, partnerships and human touch, Medi Assist has grown rapidly over the past years and is now considered a trusted name. Through strategic acquisitions, we've expanded our capabilities to serve our members not only in India but also across 141 countries worldwide.
We were exploring partners… Medi Assist really stood out because you guys had the right skills and resources that we needed as a digital-first company.

At MediBuddy, we believe in community first and company second. We passionately believe in having partners that share the same values, and Medi Assist is one of those partners. Medi Assist helped us grow our competency, while being an exceptional strategic as well as execution partner.


Always by your side, making every experience easy and smooth
General helpline: 0120 693 7372
Senior citizen helpline: 1800 419 9493